Multiple Sclerosis
August 10, 2023Cerebral Palsy
August 10, 2023
Drowning and Anoxic Brain Injury
According to the CDC, drowning is a leading cause of death in children aged 1 to 14. It is extremely dangerous as it deprives the entire brain of necessary oxygen. Often, this deprivation leads to the death of brain cells or the death of the drowning victim. In fact, brain cells begin to die within five minutes of oxygen deprivation. The parts of the brain that are most often affected are the parts that control memory, speech, and movement. That is why survivors of drowning usually suffer from deficits in memory, speech, and movement. The brain injury they experience is called anoxic brain injury or ABI.
This type of brain injury involves a temporary loss of blood supply to the brain. This is the most devastating type of brain injury and is usually seen after drowning, cardiac arrest, or birth injury. With an anoxic brain injury, all areas of the brain can be affected. However, the combination and severity is affected by a few factors.
- How long the patient is without oxygen
- How long it takes to restore normal circulation
- The adequacy of CPR
- The patient’s age
- Any pre-existing neurological or systemic diseases
- Selectively vulnerable areas of the brain
- Individual peculiarities of brain circulation and anatomy
Effects of Anoxic Brain Injury
Anoxic brain injuries can have a variety of symptoms based on the factors above. The effects will depend on which parts of the brain are affected, which are different from person to person. Some of the common symptoms are:
- Altered level of consciousness
- Decreased cognition
- Impaired motor coordination
- Gait and balance issues
- Difficulty swallowing and eating
- Sensory issues
- Impaired bowel and bladder function
Many times, patients also experience seizures. Most patients have severe impairments and are often only minimally conscious, making them totally dependent.
Benefits of Hyperbaric Oxygen Treatment for Drowning and Anoxic Brain Injury
Healing of the brain – or any part of the body – cannot take place if the tissue and cells do not receive the appropriate oxygen levels. The benefits of hyperbaric oxygen treatment for drowning are maximal when the treatment is delivered close to the time of the anoxic injury. While this is the case for all medical conditions, it is especially so for anoxic brain injuries. When delivered within three hours of the anoxic injury, HBOT can prevent as much as 90% or more of the injury, particularly the secondary more devastating component of injury which occurs when blood flow and oxygen are restored. Both the initial injury from loss of oxygen and the secondary injury when a heart beat is regained cause the loss of large amounts of both gray and white matter. The gray matter is the outer and deep parts of the brain containing brain cells and the white matter is the connecting tracts of the brain.
Why Come to Dr. Harch for Hyperbaric Oxygen Treatment of Drowning and Anoxic Brain Injury
Dr. Harch has been treating drowned children with HBOT since 1989. This experience now includes over 100 drowned patients from just 90 minutes after drowning to years after drowning. He has been summarizing the world’s literature on HBOT for anoxic brain injury in the Textbook of Hyperbaric Medicine for over twenty years. In this book chapter he showed the brain blood flow scans of two of two drowned children treated with HBOT. Dr. Harch is the world-renowned HBOT expert that people all over the world travel to see for the best treatment of drowning.
In 2016 his 41st drowned child was the now famous little girl from Fayetteville, Arkansas, Eden Carlson. With both oxygen by nasal cannula and hyperbaric oxygen Eden was able to walk and talk while her brain showed a global regrowth of lost brain tissue. Since Dr. Harch’s case study of Eden Carlson he has treated an additional 60 similar children. Treatment begins in the ICU with the intermittent dosing of oxygen, sometimes even while the child is on a ventilator.
Prior to Dr. Harch’s careful dosing of hyperbaric oxygen therapy to drowned children, there was no treatment for anoxic brain injury in adults or children. Based on the initial results with drowned children Dr. Harch has adapted his Harch ProtocolsTM to the treatment of patients with other causes of anoxic brain injury such as cardiac arrest, hanging, anesthesia accidents, suffocation, and airway obstruction in children due to grapes, beans, or other small round objects.
The results of hyperbaric oxygen treatment for drowning by Dr. Harch have gone on to far exceed the expectations of their treating doctors and neurologists. Several children are now able to stand with support, some have developed speech, and even laugh. Many parents have said that their child’s personality came back. One child in Houston is now featured in a medical school class called “Unexpected Outcomes.” If you are searching for the best treatment and results for your child’s anoxic brain injury, you have found it.
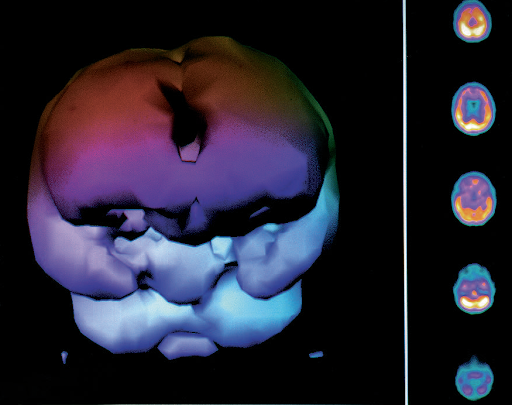
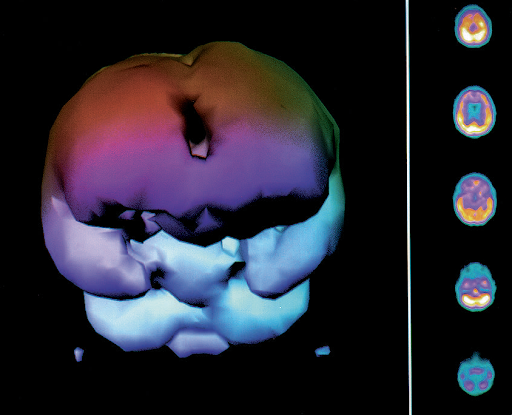
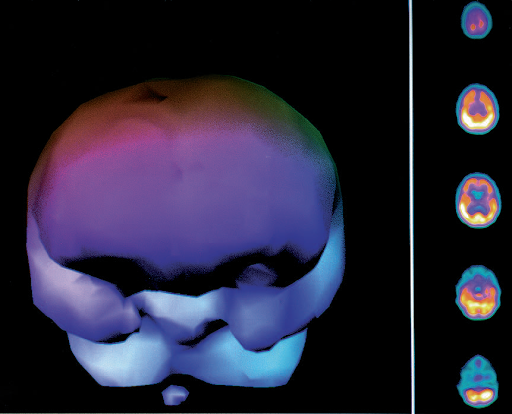
Case Study
Below are two drowned children. The first is from Dr. Harch’s initial group of 41 drowned children treated from 1989-2016. All, but one, were at least one year after drowning. This child is a 4 year old boy who was treated with HBOT in 1993, two years post-drowning. He is wheelchair bound with global deficits in cognition, speech, motor, and coordination. The first SPECT brain blood flow scan is before his first HBOT, the second is 2 hours after his first HBOT, and the 3rd is after 80 HBOTs. At the time of the 3rd brain scan this little boy had experienced an improvement in spasticity, movement of all 4 extremities, increase in trunk and head control as well as improvements in swallowing, awareness, non-verbal communication, and attention span. An HBOT-generated global increase in blood flow on the 3rd scan was responsible for all of these improvements.
Case Study #2
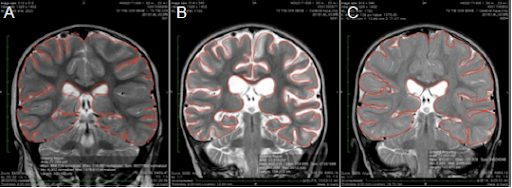
The second child is a two year old girl who was the first child in Dr. Harch’s second group of over 60 drowned children, nearly all of whom were treated within 6 months of drowning from 5/2016 to present. Her case was published in Medical Gas Research in 2017 (https://www.medgasres.com/temp/MedGasRes72144-6908434_191124.pdf). Her MRI scans below show a global loss of brain tissue one month after her drowning and a near complete regrowth and restitution of brain volume after normobaric oxygen by nasal cannula and hyperbaric oxygen. At the time of initiation of the nasal cannula oxygen she was a thrashing semi-conscious little girl. At the time of the final MRI she was walking and talking (see the videos in the link above).
The MRI slices below are what are called coronal slices, a view from the top of the head to the bottom. In each slice you are looking directly at this little girl. The left side of the image is the right side of her head. MRI scan A is 3 days after drowning. MRI scan B is 31 days after drowning where there has been a 12.3% loss of brain tissue, seen as increased white color on the scan (white is the cerebrospinal fluid or water of the brain). MRI scan C is 27 days after her 40th HBOT or 162 days after drowning. This is normally the time when one sees near-maximal loss of brain tissue. Instead, she has experienced a 13.9% increase in brain tissue.
Supportive Research and Information